The Impact of Nursing: Nurses Transforming Patient Care Outcomes
Nurses play a crucial role in influencing a patient’s recovery journey, often more than most people realize. Their presence fosters comfort, safety, and confidence throughout every phase of care. A patient may arrive at the hospital feeling anxious, but with the steady support of a nurse, that experience can transform into one of reassurance.
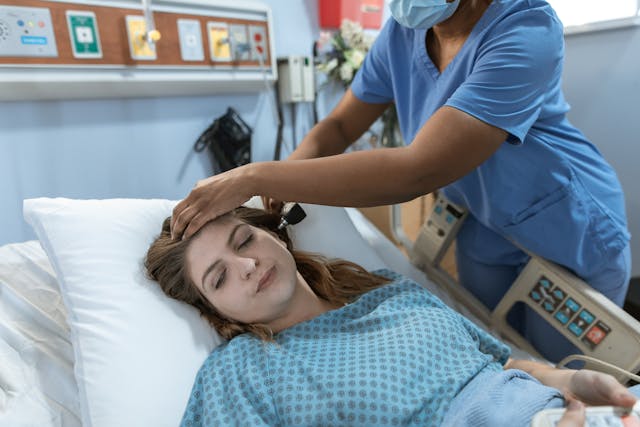
Image Source
The integration of clinical expertise and emotional intelligence enhances outcomes across various health conditions. Each interaction bears significance, and every choice made by nurses contributes to healthier and more stable results. Their responsibilities extend far past routine tasks, showcasing the profound impact they have on the patient’s journey.
The Essential Role of Nurses in Contemporary Healthcare
Healthcare teams rely on nurses to keep patient needs at the forefront. Nurses notice subtle changes in patients that might go unnoticed in busy clinical settings. Because patients spend most of their time with nursing staff, trust often develops organically during routine care, creating a supportive atmosphere throughout treatment.
Nurses facilitate discussions, clarify care plan steps, and encourage patient engagement in their recovery. These regular interactions provide a framework that transforms potentially confusing or overwhelming moments into manageable experiences. When patients feel supported by their nurses, the care received becomes more cohesive.
The Human Element That Enhances Patient Recovery
Healing thrives in a compassionate environment. Patients tend to improve when communication is transparent and heartfelt, a setting that nurses cultivate with their consistent presence and attentive listening. Patients who feel acknowledged are more likely to share crucial information about their symptoms, concerns, and anxieties.
These insights are vital in shaping treatment decisions and reinforcing collaboration between patients and providers. Much of this progress stems from strong interpersonal skills, as effective nursing fosters connections that alleviate stress and bolster confidence. Approaching patients with patience and clarity enhances comfort and encourages cooperation throughout their recovery. Skills such as empathy, effective communication, collaboration, and problem-solving complement effective nursing care and lead to positive patient outcomes.
The Role of Clinical Judgment in Treatment Success
Clinical judgment is key as nurses assess rapidly changing situations. A minor change in a patient’s breathing, skin color, or alertness can indicate significant issues, and a well-prepared nurse can interpret such signals effectively. Early detection often helps prevent complications and allows for timely interventions from physicians before conditions escalate.
Nurses evaluate each situation using a blend of experience, education, and evidence-based intuition. Their consistent decision-making influences the efficacy of treatment strategies. Patients experience benefits when nurses react swiftly, articulate concerns effectively, and assist in coordinating next steps. Strong clinical judgment enhances patient safety and significantly eases their path toward recovery.
The Significance of Patient Education and Advocacy
Providing clear explanations allows patients to understand the importance of each aspect of their care. Nurses address inquiries that arise during treatment, fostering confidence. Patients are more inclined to adhere to instructions when the underlying reasoning is clear and relatable. Advocacy plays a crucial role in ensuring patient needs remain prioritized.
Nurses advocate when a treatment appears inappropriate or when a patient expresses discomfort or uncertainty. This support upholds patient rights and empowers them to participate in care decisions. Informed and respected patients are more likely to take ownership of their recovery, leading to improved long-term results.
The Role of Nurse-Led Coordination in Multidisciplinary Care Teams
Effective care hinges on seamless communication between providers. Nurses bridge information among specialists, doctors, therapists, and family members, clarifying the patient’s status for all involved. This coordination helps minimize misunderstandings that could hinder treatment or add unnecessary stress.
Patients face fewer interruptions when nurses organize updates, clarify directions, and promote consistent follow-through. Healthcare team members depend on nurses to align care plans, especially in interdisciplinary settings. This ongoing coordination helps patients navigate their recovery stages more smoothly, enhancing overall outcomes.
The Influence of Cultural Competence on Care Quality
Patients come with diverse beliefs, customs, and expectations shaped by their backgrounds and experiences. Cultural competence enables nurses to engage with each patient respectfully, making care more impactful when communication aligns with a patient’s values and preferences.
A patient who feels their cultural background is recognized is likely to engage more openly during assessments and discussions. This engagement provides nurses with clearer insights into symptoms, lifestyle influences, and potential treatment barriers. Cultural awareness also helps avoid misunderstandings that could impede progress.
The Resilience Nurses Demonstrate in High-Stress Situations
Medical emergencies challenge not just clinical skills but emotional strength. In critical moments, nurses stabilize the environment by providing calm, clear direction, enabling teams to respond swiftly and efficiently. Their presence calms patients who may be overwhelmed by fear or discomfort. A composed nurse can reassure family members, guide patients through unfamiliar procedures, and assist colleagues in maintaining steady communication.
These competencies develop over years of experience and exposure to various scenarios. Patients benefit from this calmness, as it fosters a sense of safety amid uncertainty. Families also find reassurance when nurses explain the situation and outline the team’s objectives.
The Long-Term Value of Nurse-Patient Relationships
Robust relationships do more than enhance the care environment; they positively influence outcomes long after the hospital stay. Many patients retain vivid memories of supportive interactions with nurses that shape their approaches to future health decisions.
Enduring trust often encourages patients to adhere to medication regimens, attend follow-up appointments, and adopt healthier lifestyles. Nurses provide guidance during lifestyle changes, offer encouragement during setbacks, and clarify realistic expectations for progress. These lasting connections transform brief periods of care into ongoing motivation for improved health.
Nurses significantly impact patient outcomes through a unique combination of expertise, communication, and compassion. Their ability to recognize subtle changes, clarify complex concepts, and shepherd patients through challenging experiences influences nearly every aspect of care. Trust is built when nurses listen attentively and respond clearly, ultimately enhancing recovery.
Additionally, smooth communication aids in collaboration among care teams, ensuring that every component of the care plan aligns with the patient’s objectives. Cultural sensitivity, emotional resilience, and relationship-building complement a skill set that extends well beyond technical duties. Positive patient outcomes often hinge on the time a nurse invests in connection, observation, and deliberate action.
Add Your Comment Cancel reply
This site uses Akismet to reduce spam. Learn how your comment data is processed.